
Echocardiography predicts death in patients with acute COVID-19 infection (WASE-COVID study).
- | By Ultromics
Karagodin et al, J Am Soc Echocardiogr. 2021.
Karagodin et al, ASE 2021.
 |
Why it matters EchoGo Core is predictive of patient outcomes and is proven to be more superior than manual alone. Myocardial Strain is also a better prognostic measure than EF. Automated GLS with EchoGo Core can be used alongside EF to better detect heart failure. |
Introduction:
The novel severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) virus which has led to the global Coronavirus disease-2019 (COVID-19) pandemic is known to adversely affect the cardiovascular system through both direct and indirect mechanisms.
In this international, multi-center study conducted by the World Alliance Societies of Echocardiography (WASE), we aim to determine the clinical and echocardiographic phenotype of acute cardiac disease in COVID-19 patients, using FDA-cleared EchoGo Core, to explore phenotypic differences in different geographic regions across the world, and to identify which echocardiographic parameters are most predictive of early clinical outcomes such as heart failure.

Methods:
We studied 870 patients with acute COVID-19 infection from 13 medical centers in four world regions (Asia, Europe, United States, Latin America) who had undergone transthoracic echocardiograms (TTEs). Clinical and laboratory data were collected, including patient outcomes during their initial hospitalization.
Anonymized echocardiograms were analysed with EchoGo Core to calculate left ventricular (LV) volumes, ejection fraction (EF), and LV global longitudinal strain (GLS).

 |
EchoGo Core is FDA-cleared and backed by real-world validation. To learn more, download our whitepaper on EchoGo. |

Significant regional differences were noted in terms of patient co-morbidities, severity of illness, clinical biomarkers, LV and RV echocardiographic metrics. Overall, 46.2% of the patients were in the intensive care unit, 27.1% were on a ventilator and in-hospital mortality was 22.2%. Predictors of mortality in a multivariate analysis were age (OR 1.12 [1.05, 1.22], p = 0.003), previous lung disease (OR 7.32 [1.56, 42.2], p = 0.015), LV GLS (OR 1.18 [1.05, 1.36], p = 0.012), LDH (OR 6.17 [1.74, 28.7], p = 0.009), and RV FWS (OR 1.14 [1.04, 1.26], p = 0.007).
LV and RV dysfunction are common manifestations of acute COVID-19 illness and portend a poor prognosis. Age at presentation, previous lung disease, lactic dehydrogenase (LDH) level, LVGLS, and RVFWS were independently associated with in-hospital mortality. Regional differences in patient phenotype highlight the significant differences in echocardiographic utilization and risk in these patients.
Key Results:
- 10 of the 13 medical centers performed limited cardiac exams as their primary COVID in-patient practice, and just 3 out of the 13 centers performed comprehensive exams.
- In-hospital mortality rates varied by region, 11% in Asia, 19% in Europe, 27% in Latin America, and 26% in U.S.
- Left ventricular longitudinal strain (LV LS), right ventricle free wall strain (RV FWS), in addition to age at presentation, lactic dehydrogenase (LDH), and previous lung disease were independently associated with mortality, while left ventricle ejection fraction (LVEF) was not.
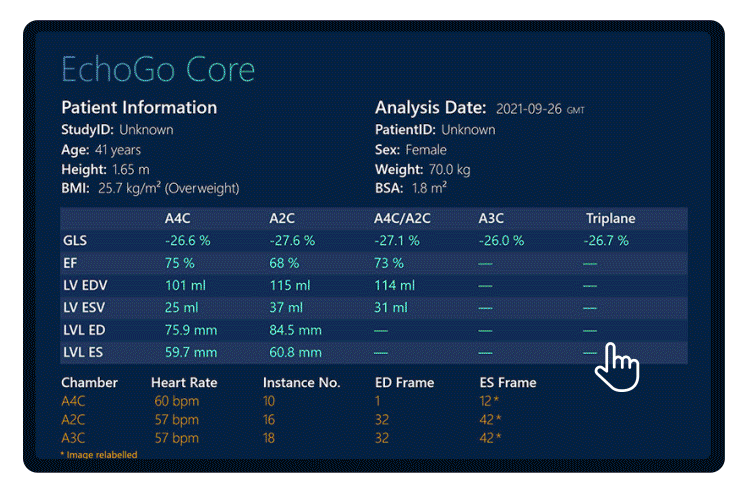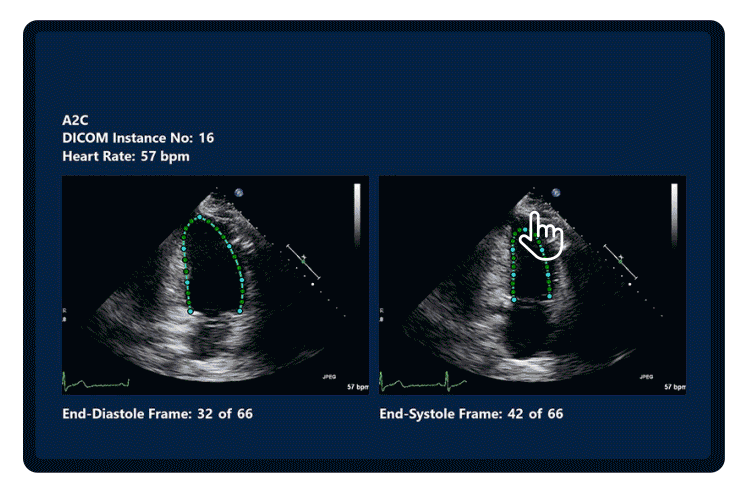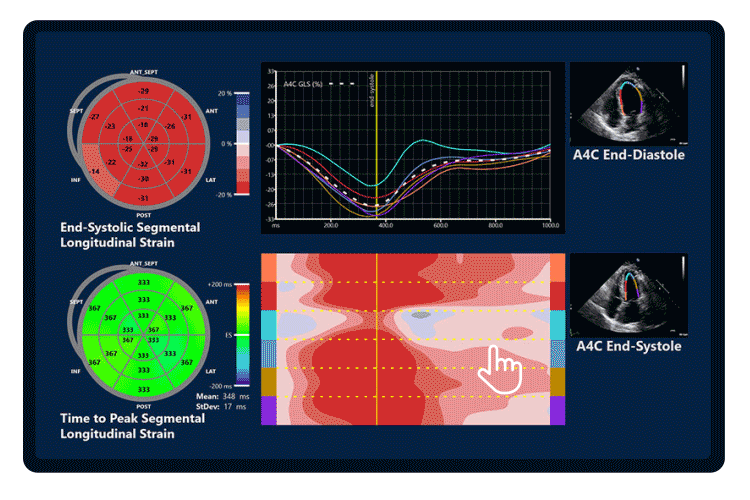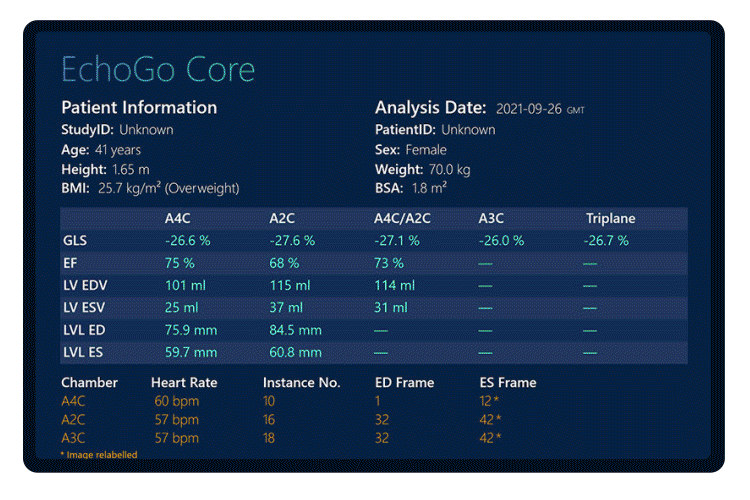
- Fully automated quantification of LVEF and LVLS using AI minimized variability.
- AI-based LV analyses, but not manual, were significant predictors of in-hospital and follow-up mortality.
Conclusion:
Left ventricular longitudinal strain (LV LS) was independently associated with mortality, while left ventricle ejection fraction (LVEF) was not. Fully automated quantification of LVEF and LVLS using AI minimized variability.
AI-based LV analyses, but not manual, were significant predictors of in-hospital and follow-up mortality.
See full publication: https://www.onlinejase.com/article/S0894-7317(21)00483-1/fulltext
