2022 AHA/ACC/HFSA heart failure guidelines emphasize prevention
- | By Ultromics
- Articles, Heart Failure

|
Professor Paul Leeson Professor of Cardiovascular Medicine at the University of Oxford and co-founder of Ultromics. |
New industry Heart Failure (HF) guidelines were published on April 01 2022, and launched at the American College of Cardiology (ACC) annual session in Washington, D.C. [1]
The update was a joint effort by experts from the American College of Cardiology (ACC), the American Heart Association (AHA), and the Heart Failure Society of America (HFSA).
The new guidelines help healthcare providers treat patients who have heart failure as well as patients who are at risk for the disease.
The last full set of HF guidelines published by these societies dates back to 2013, with a “focused update” released in 2017. Of note, the European Society of Cardiology (ESC) released its newest heart failure guidelines last fall during the ESC Congress. There are many areas of overlap between the two documents.
Professor Paul Leeson shares key takeaways from the new guidelines.
Summary of the Guidelines
Key aspects of the 2022 heart failure guidelines include an increased focus on prevention, new recommendations for patients who have heart failure with preserved ejection fraction (HFpEF) or amyloidosis and include some newer treatment options based on disease progression and comorbidities.
“American adults have a 20% risk of developing heart failure in their lifetime, so prevention is key” said Professor Paul Leeson. He continued: “The guidelines redefine heart failure stages to focus on prevention and put emphasis on care coordination, in the hope that millions of people who are at risk for heart failure might be able to stop the disease progression and improve their quality of life”.
Heart Failure StagesThe American Heart Association (AHA) classifies the levels of heart failure as:
|
Key Highlights from the Guidelines:
New Staging of HF
The guideline updates include a new focus on preventing HF in people who are showing early signs of “pre-heart failure,”. One focus was the prevention of heart failure through optimizing blood pressure control and adherence to a healthy lifestyle.
The societies revised the ACC/AHA stages of HF — from stage A to stage D — to emphasize the development and progression of the disease, with advanced stages indicating a more serious disease and reduced survival rate. The updated staging system is as follows:
- Stage A: At Risk for HF. No symptoms or clinical signs of HF, but the patient has one or more risk factors (i.e., high blood pressure, diabetes, obesity, family history, etc.).
- Stage B: Pre-HF. No symptoms of HF, but clinical evidence is present (i.e., reduced ejection fraction, heart muscle enlargement, contraction abnormalities, etc.)
- Stage C: Symptomatic HF. Structural heart disease with current or previous symptoms of heart failure.
- Stage D: Advanced HF. HF with symptoms that interfere with daily life is difficult to control and results in recurrent hospitalizations despite treatment.
Therapeutic interventions in each stage aim to modify risk factors (stage A), treat risk and structural heart disease to prevent HF (stage B), and reduce symptoms, morbidity, and mortality (stages C and D).
Of note is the number of people with Stage A heart failure. Approximately 121.5 million people in the U.S. with high blood pressure, 100 million experience obesity, and 28 million with diabetes, which suggests that a significant proportion of the U.S. population is categorized as stage A, and is at risk for HF.
SGLT-2
For the first time, we have therapy, and consideration of other therapies, that improve outcomes in patients with heart failure with preserved EF.
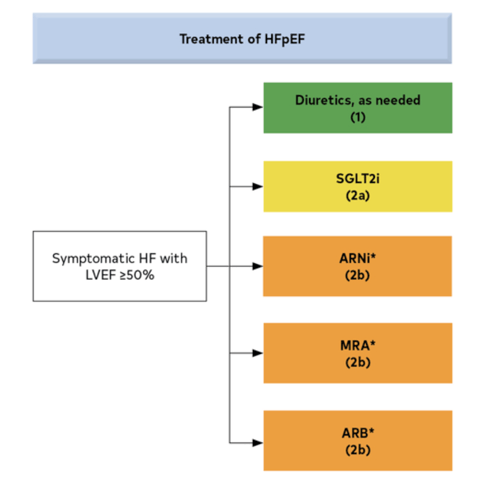
Most existing treatments are aimed at targeting reduced ejection fraction (HFrEF) patients. That leaves potentially 50% of patients with preserved (HFpEF) or midrange (HFmEF) ejection fraction with fewer treatment options.
The guidelines have addressed this commonly overlooked group by suggesting SGLT2 inhibitors be used as part of a four-drug class approach for those with symptoms. This new class of medications can be used to reduce complications, hospitalizations, and death caused by heart failure for patients with HFmrEF and HFpEF. The SGLT-2 inhibitor has been demonstrated in studies to reduce the risk of death and lower the risk of hospitalization by 30%.
Experts also now recommend a greater focus on prevention for patients at risk of heart failure or with evidence of pre-heart failure to include ensuring good blood pressure control (less than 120/80mmHg) and consideration of SGLT-2 inhibitor (SGLT2) for those with diabetes or who are at high cardiovascular risk.
New classification of Ejection Fraction
The updated heart failure guidelines also made changes to the four left ventricular ejection fraction (LVEF) classifications.
The updated levels of ejection fraction (normal range is 50%–55%) are:
- HFrEF (reduced ejection fraction): less than or equal to 40%
- HFimpEF (improved ejection fraction): improved from less than 40% to above 40%
- HFmrEF (mildly reduced ejection fraction): between 41%–49%
- HFpEF (preserved ejection fraction): above 50% but with increased filling pressures
Key Takeaways
|
How Ultromics Helps Detect Heart Failure
The new HF guidelines highlight how effective and efficient echocardiographic left ventricular (LV) function is to guide treatment decisions for patients with heart failure. Ultromics is an AI-powered platform which can be connected through the cloud to automate LV insights and provide reports whenever an echocardiogram is performed. The technology offers significantly improved heart failure detection by automating ejection fraction (EF), volumes, and –notably – global longitudinal strain (GLS), with zero variability.
Global longitudinal strain (GLS) has become a recommended measurement for detecting heart failure and HFpEF, which occurs in 50% of HF patients. The European Society of Cardiology (ESC) heart failure guidelines, published in December 2021, suggested “GLS is an early indicator of HF and adverse outcomes”. The AHA/ACC/HFSA HF guidelines also suggest a GLS<16% indicates abnormal left ventricular filling pressures, so there is even more importance placed upon, not only adding GLS measurements to regular reporting practices but also ensuring that these measurements can be performed with minimal variability and in a timely manner – two issues which have halted the wider use of GLS in clinical practice.
Ultromics' revolutionary use of AI and cloud capabilities can automate GLS and EF with speed, accuracy, and zero variability. The platform replaces legacy on-premises software, so clinicians can benefit from streamlined care which holds greater flexibility and accelerated innovation.
These new Heart Failure Guidelines illustrate that now, more than ever, clinicians and their patients can significantly benefit from accurate detection and earlier prevention through echocardiography. [1]
References:
- Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Journal of the American College of Cardiology. 2022;79:263-421
- American College of Cardiology : https://www.acc.org/
- ACC, AHA, HFSA Issue Heart Failure Guideline [Internet]. American Heart Association. 2022
- Nagueh SF, Smiseth OA, Appleton CP, Byrd BF, Dokainish H, Edvardsen T, et al. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography. 2016;29:277–314.
- Karagodin I, Carvalho Singulane C, Woodward GM, et al. Echocardiographic Correlates of In-Hospital Death in Patients with Acute COVID-19 Infection: The World Alliance Societies of Echocardiography (WASE-COVID) Study. Journof the American Society of Echocardiography. 2021;34:819–30
Curious about upcoming research and innovation?
Sign up to hear about the latest news.